When I started out on this journey, having my daughter receive the diagnosis of Childhood Apraxia of Speech was devastating. Unlike other parents who might have needed it explained or who turned to google and realized it is a lifelong neurological disorder, being an SLP I already knew that. My mind flashed to two boys I treated prior to Ashlynn when I was a school SLP, who both entered Kindergarten nonverbal and I was terrified.
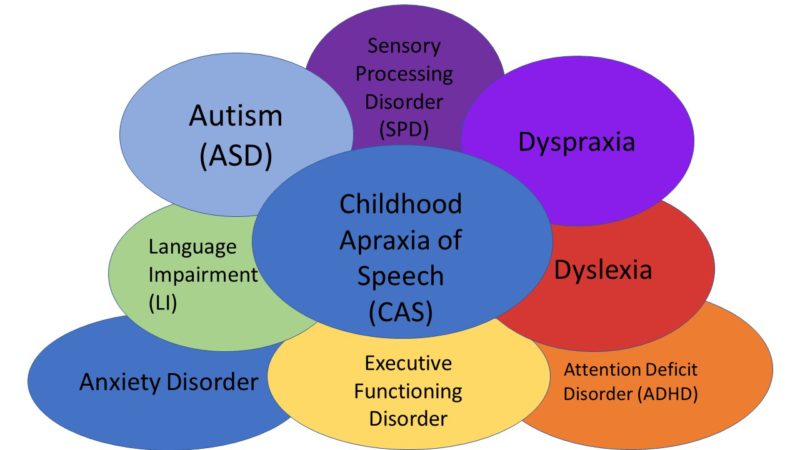
After I threw myself a pity party, I picked myself up determined to attack the beast named apraxia. At the time as we were going through it, I did not fully grasp as I do now, the fact that most kids with apraxia will not only hold that one label. I did not fully realize that most kids with apraxia, a neurological speech disorder, will also have co-morbid neurological disorders as well.
As a professional SLP specializing in the field, I have a current private practice caseload of around 35 kids. There is not one who doesn’t have another co-morbid condition. Friends, I have to repeat that because it is important. There is not ONE who only has apraxia.
I feel now like this is an important topic to discuss because I don’t know about other parents, but for me I would have wanted to know up front that a diagnosis of CAS meant I was going to be dealing with more than CAS for the long haul.
Why? What does it matter? You take each diagnosis day by day right?
I struggle with this. Part of me agrees but then part of me just wishes I had known the statistics were as high as they were for the chances that my daughter would have dyslexia, or ADHD, or SPD. I say this because honestly, had I just known up front all of that was a possibility, I could have:
1. Been more vigilant and more proactive about potential comorbidities
2. Not been so devastated each time a new one popped up.
I know it’s a little too young to diagnose ADD, but I hope to God she doesn’t have that too. She doesn’t deserve this..any of this.
In the post on Dyslexia I wrote:
In that moment, my dear readers, I had the same gut feeling I had when that SLP told me back when Ashlynn was 2:11 “Laura this is apraxia.” In that moment, that article told me, “Laura, this is dyslexia.” I started to cry at the end of that article. Damnit. I missed it again. I missed another OBVIOUS dx in my OWN daughter. Why does this keep happening?? What good was all my training and experience when I’m not applying it to my OWN baby??
Ashlynn has a slew of other diagnoses as well, and EACH time I went through this process AGAIN. I had to relive the pain of a diagnosis AGAIN. I guess I can’t say if the pain would have been any less had I known all of these diagnoses were more of probabilities that possibilities, but I honestly think it wouldn’t have made each new diagnosis as gut wrenching.
I was talking to Lynn Carahaly the other day, creator of the Speech EZ program for apraxia and apraxia expert out of Arizona, and she said the following,
Over my career specializing in the disorder, I definitely feel apraxia is rarely the primary issue, rather a sequela to a bigger picture. The problem is SLP’s and parents are so focused on the speech and not looking at the big picture in early development. There is this thinking that if we could just overcome the apraxia, everything will be OK.
I let out a big sigh after reading that. Anyone else who felt that way, will you raise your hand with me? I fell into that category. I was so convinced if we could just fight and beat this beast called apraxia, everything else was going to be okay, and man I was wrong. Consequently, each new diagnosis brought this sense of total indignation. We fought apraxia and WON!! Why now did she have to deal with something else?
I take a different approach now with my clients. I am completely honest and transparent about the potential for co-morbid issues. In fact, I told one mother the other day,
Your daughter is at risk for dyslexia. I recommend that for now we operate under the assumption she might have it and get her started early with pre-literacy and phonemic awareness activities; and if she doesn’t have dyslexia, we celebrate.
I’m just giving parents, and now all of you, what I personally would have wanted to hear. Lynn is right, and that’s why her program incorporates so many pre-literacy elements. Let’s start looking at apraxia as more than just a speech disorder, and let’s celebrate if the child did indeed only have apraxia. Once I started connecting with parents of kids who have global apraxia, only then did I realize every child with global apraxia had a co-morbid diagnosis of ADHD. The same was true when I found the apraxia-kids facebook group and realized just how many kids with apraxia also had Sensory Processing Disorder! Oh, and when I found out that and started talking to my global apraxia friends, just how many kids with global apraxia had a similar and rare presentation of sensory processing disorder in that they had a high tolerance for pain and an “under-responsive” tactile system!
Parents and professionals, the moral of the story is this. In most cases, apraxia is just a foreshadowing of additional neurological conditions to come. There are many, MANY, combinations it would be impossible to predict at that initial CAS dx. Dr. Ruth Stoeckel did a talk at one apraxia conference titled “Co-Occurring Diagnoses: Other Letters that may go with CAS.” There are MANY other conditions that can and DO go with CAS. I think it benefits parents and professionals to know we are dealing with just the beginning of what is probably a very bigger picture.
Resources:
Duchow, H., Lindsay, A., Roth, K., Schell, S., Allen, D., & Boliek, C. A. (2019). The co-occurrence of possible developmental coordination disorder and suspected childhood apraxia of speech. Canadian Journal of Speech-Language Pathology and Audiology.
Iuzzini-Seigel, J. (2019). Motor Performance in Children With Childhood Apraxia of Speech and Speech Sound Disorders. Journal of Speech, Language, and Hearing Research, 62(9), 3220-3233.
Langer, N., Benjamin, C., Becker, B. L., & Gaab, N. (2019). Comorbidity of reading disabilities and ADHD: structural and functional brain characteristics. Human brain mapping, 40(9), 2677-2698.
Lewis, B. A., Freebairn, L. A., Hansen, A. J., Iyengar, S. K., & Taylor, H. G. (2004). School-age follow-up of children with childhood apraxia of speech. Language, Speech, and Hearing Services in Schools.
Miller, G. J., Lewis, B., Benchek, P., Freebairn, L., Tag, J., Budge, K., … & Stein, C. (2019). Reading Outcomes for Individuals With Histories of Suspected Childhood Apraxia of Speech. American journal of speech-language pathology, 1-16.
Teverovsky, E. G., Bickel, J. O., & Feldman, H. M. (2009). Functional characteristics of children diagnosed with childhood apraxia of speech. Disability and Rehabilitation, 31(2), 94-102.

Laura Smith, M.A. CCC-SLP is a 2014 graduate of Apraxia Kids Boot Camp, has completed the PROMPT Level 1 training, and the Kaufman Speech to Language Protocol (K-SLP). She is the author of Overcoming Apraxia and has lectured throughout the United States on CAS and related issues. Currently, Laura is a practicing SLP specializing in apraxia at her clinic A Mile High Speech Therapy in Aurora, Colorado.